Alessi to deliver keynote at The Concussion Conference
For immediate release
Board-Certified Neurologist Dr. Anthony Alessi to deliver keynote at The Concussion Conference at Quinnipiac University Sept. 24
Hamden, Conn. – Sept. 2, 2014 – Dr. Anthony Alessi, a board-certified neurologist, will be the keynote speaker at “The Concussion Conference 3.0: Return to Learn then Return to Play,” which will take place from 8 a.m. to 4:30 p.m. on Wednesday, Sept. 24, at the Center for Medicine, Nursing and Health Sciences on the North Haven Campus at Quinnipiac University, 370 Bassett Road, North Haven.
The conference, which is open to the public, is designed primarily for school administrators, athletic directors, coaches and their staffs and clinical and academic staffs, including guidance counselors, nurses, social workers, athletic trainers and teachers.
Conference Organizer Katherine Snedaker, founder, advocate and researcher, PinkConcussions.com, SportsCAPP.com and TheConcussionConference.com said, “To help schools update their policies and use best practices for the 2014-15 school year, the top medical, academic, legal and athletic concussion experts will assemble at Quinnipiac to present this new information to school nurses, athletic directors, athletic trainers and administration.”
Alessi, an associate clinical professor of neurology at the University of Connecticut, will deliver his keynote address “Sports Concussions: What Do We Really Know?” at 8:15 a.m. He will discuss recent sports concussion media hype and sort out the facts, myths and educated guesses by experts in the field. He will cover the current risks of playing sports and the possible long-term effects of playing. He also will help nurses, educators and athletic departments to learn how to base their school concussion policies on scientific data and not unwarranted hype.
Alessi will be among 14 conference speakers who will present on a variety of concussion-related issues, including the 2014 Connecticut Concussion Law, which now affects all K-12 schools in the state. The speakers also will discuss research-based best practices for treating those with concussions, creating an efficient and streamlined school concussion management team, educating parents and players about concussions, and planning for academic adjustments during weeks one through three and beyond.
In addition to Alessi and Snedaker, the conference speakers include: Fred Balsamo, executive director of the Connecticut Association of Athletic Directors; Sarah Bullard, neuropsychologist at Gaylord Center for Concussion Care; James Doran, president of the Connecticut Athletic Trainers’ Association; David Johnson of DKJ Sports Medicine Associates; Dr. Michael Lee, of Concussion Specialists of Connecticut; Suzanne Levasseur, supervisor of health services, Westport Public Schools; Patricia McDonough-Ryan, pediatric neuropsychologist, Concussion Center of Fairfield County; Karissa Niehoff, executive director of the Connecticut Association of Schools, Connecticut Interscholastic Athletic Conference; John Pizzi, director of athletics, Riverdale County School; T.J. Quinn, investigative reporter, ESPN; Paul Slager, attorney, brain injury litigation, Silver, Golub & Teitell LLP; and Dr. David Wang of Elite Sports Management, who also is the team physician at Quinnipiac.
“I am thrilled to have this dream team of top experts to present at this conference to the schools on the latest medical, academic, legal and athletic concussion information,” Snedaker said. “When schools improve how they manage concussions, schools lower their liability risk and to help students heal faster to return to class, friends and sports.”
The Gaylord Center for Concussion Care and Quinnipiac University are conference sponsors.
To register, please visit www.TheConcussionConference.com.
Quinnipiac University's Center for Medicine, Nursing and Health Sciences is home to the School of Health Sciences, the Frank H. Netter MD School of Medicine and the School of Nursing. The facility includes 325,000 square feet designed for collaborative learning for students pursuing degrees in medicine, nursing and the health professions. The three schools are united not only in the same complex but by the same mission: to graduate medical and health care practitioners who will be the driving force for a more collaborative, economical and efficient health care system.
Quinnipiac is a private, coeducational, nonsectarian institution located 90 minutes north of New York City and two hours from Boston. The university enrolls 6,500 full-time undergraduate and 2,500 graduate students in 58 undergraduate and more than 20 graduate programs of study in its School of Business and Engineering, School of Communications, School of Education, School of Health Sciences, School of Law, Frank H. Netter MD School of Medicine, School of Nursing and College of Arts and Sciences. Quinnipiac consistently ranks among the top regional universities in the North in U.S. News & World Report’s America’s Best Colleges issue. The 2014 issue of U.S. News & World Report’s America’s Best Colleges named Quinnipiac as the top up-and-coming school with master’s programs in the Northern Region. Quinnipiac also is recognized in Princeton Review’s “The Best 377 Colleges.” The Chronicle of Higher Education has named Quinnipiac among the “Great Colleges to Work For.” For more information, please visit www.quinnipiac.edu. Connect with Quinnipiac on Facebook at www.facebook.com/quinnipiacuniversity and follow Quinnipiac on Twitter @QuinnipiacU.
###
Media Contact:
John W. Morgan, associate vice president for public relations, Quinnipiac University
(203) 582-5359 (office)
(203) 206-4449 (cell)
http://facebook.com/quinnipiacuniversity @QuinnipiacU | @jwmorganjr http://quinnipiac.wordpress.com
http://gplus.to/quinnipiacuniversity http://www.quinnipiac.edu
The Unofficial Summary of the #TheFIFA5 Lawsuit
 This summary is based on information posted on the Hagens Berman S Shapiro LLP website and is my unofficial review of the lawsuit I have hash tagged as #TheFIFA5. NOTE: I am not a lawyer, and am merely outlining the suit as I read it. I welcome comments and thoughts.
On August 27, 2014, a Class-Action Lawsuit Filed Against FIFA, U.S. Youth Soccer Over Concussions made headlines. This lawsuit pits three mothers and two female college students vs FIFA, soccer’s worldwide governing body—the Fèdèration Internationale de Football Association (FIFA)—and affiliated soccer organizations in the United States
This summary is based on information posted on the Hagens Berman S Shapiro LLP website and is my unofficial review of the lawsuit I have hash tagged as #TheFIFA5. NOTE: I am not a lawyer, and am merely outlining the suit as I read it. I welcome comments and thoughts.
On August 27, 2014, a Class-Action Lawsuit Filed Against FIFA, U.S. Youth Soccer Over Concussions made headlines. This lawsuit pits three mothers and two female college students vs FIFA, soccer’s worldwide governing body—the Fèdèration Internationale de Football Association (FIFA)—and affiliated soccer organizations in the United States
- US Soccer Federation
- U.S. Youth Soccer + American Youth Soccer (over 3 US million child and adolescent soccer players)
Note: In 2013, FIFA reported $1.386 billion in revenue. The 2014 World Cup brought FIFA $1.2 billion from U.S. broadcasters. This lawsuit states FIFA has failed to enact the policies and rules needed to protect soccer players. FIFA and the others mentioned…
- Failed to adopt effective policies to evaluate and manage concussions, at all levels of the game
- Lacked of effective policies poses a greater danger to women and children players, who may more vulnerable to traumatic and long-lasting brain injury
- Ignored medical community called for changes over a decade ago
- Ignored simple, best-practice guidelines, which have been updated three times since the initial international conference on concussions (FIFA even hosted)
FIFA has made progress…
- With Concussion Marketing and policy materials, which tout a commitment to player safety
- By implemented policies to address other health threats (cardiac arrest and performance-enhancing drugs)
- Hosted 2012 concussion conference that updated concussion guidelines
This lawsuit demands FIFA and others mentioned…
- Implement up-to-date guidelines for detection of head injuries
- Implement up-to-date RTP after a concussion
- Regulation of heading by players under 17 years old
- Eliminate heading under 14 years old age groups
- Implement a rule change to permit substitution of players for medical evaluation purposes. (Currently, FIFA rules generally allow only three substitutions per game with no clear provision for head injuries. If an athlete bleeds, even from a scrape, removal is required, but no similar rule exists for concussions. FIFA provides no guidance on substitutions in youth games in the U.S.)
- Implement medical monitoring for soccer players who received head injuries in the past
photo source: source: http://screamer.deadspin.com/concussed-christoph-kramer-cant-really-remember-world-1604847904
The Concussion Conference: Connecticut
The new 2014 CT Concussion Law applies to students K-12 as well as athletes.
Is your school ready with updated policies/practices for the 2014-15 year?
The Concussion Conference: 2014 Connecticut Concussion Law & Research-Based Best Practices for K-12 Schools
Wednesday, Sept 24, 2014 Hosted by Quinnipiac University Medical School, North Haven Campus Produced by Katherine Snedaker, LMSW Sponsored by Gaylord Center for Concussion Care
Register at TheConcussionConference.com - NY and AZ Conferences in 2015
Opening Remarks ESPN’s TJ Quinn
Keynote “Sports Concussions: What do we really know?” Anthony Alessi, MD
Presentations from Medical, Academic, Legal and Athletic Concussion Experts for all levels of school staff
Administration Superintendents, Principals, Headmasters, Business Managers, ADs, Heads of Pupil Services Athletic Dept. Staff ADs, ATs, Coaches Clinical and Academic Staff School RNs, Guidance Counselors, Psychologists, Social Workers, ATs, Teachers
Schedule All Participants can come partial, half or full day
Continental Breakfast 7:45 AM Administration Sessions 8 AM -10 AM Athletic Dept. Sessions 8 AM-12 PM Clinical/Academic Sessions 8 AM-4:30 PM
Questions Katherine Snedaker 203-984-0860 Katherine@SportsCAPP.com
Pink Concussions at American Academy of Neurology Sports Concussion Conference
|
||||||||||||||||||
|
Guest Blog: Concussions: The Gender Differences
 By Arleigha Cook as a Guest Blogger
By Arleigha Cook as a Guest Blogger
“You just have to get back out there.”
“That’s not a concussion headache. That’s just a hunger headache.”
“Just start exercising. That helped me.”
These quotes are all from conversations I had regarding concussions. At a glance, I’m sure you sense a pattern. Each of the above is a well-intentioned piece of advice, but, characterized by the notorious word “just,” each of these replies is incurably dismissive. In fact, they all tore at something inside me, as if the speaker took a look at me, saw my hope for validation of my concussion symptoms, and then pulled out the carpet from underneath me with an overtly simplistic suggestion of a quick recovery method that I should have seen before.
Interestingly, these people were brain injury survivors themselves. And they were all male.
Hearing from another concussed individual that I should have been doing something different from the get-go – especially something as simple as beginning to exercise or just “getting back out there” was devastating. To this day, each time I hear a suggestion of that nature, I sigh and push away an emotional reaction. It was especially invalidating to hear from one of my friends (a skier and rugby player who had previously sustained three concussions) who said, “That’s not a concussion headache. That’s just a hunger headache.” To me, the pain of a “hunger headache” is the same as that of a “concussion headache.” A hunger headache is a concussion headache. Likewise, I have not been able to exercise without almost immediately experiencing concussion symptoms for over a year and seven months – I’m sure you can imagine how quickly I dismissed his “advice.”
These interactions got me thinking: men seem to recover from concussions more quickly than women do. And even when they don’t, they seem to have a dismissive or nonchalant attitude about their recovery. So I started researching that idea, but only came across studies suggesting the contrary. For example, a recent study published in the journal Radiology suggests that men actually take longer to recover from a concussion than women (see a Huffington Post article about the study here).While I have always thought I sounded like a hypochondriac, my tendency to air on the safe side may actually prove more beneficial than the laissez faire attitudes of concussed males. More than a few times I’ve come across men with concussion experience who think I’m exaggerating my symptoms (hence, “That’s not a concussion headache. That’s a hunger headache.”). The study featured in the Huffington Post article above even found, through diffusion tensor imaging (DTI – a form of MRI), that men seem to sustain significantly more abnormalities in a particular area in the white matter of their brains, otherwise known to scientists as the Uncinate Fasciculus.
Is this related to a basic genetic difference between men and women? Is it the significant change to the Uncinate Fasciculus that causes male concussion patients to underestimate the time, importance, and attention their brains need in order to recover more quickly and effectively? Presently, it’s hard to say.
My observations – which largely consist of college-age male athletes who receive concussions from football, lacrosse, and soccer – indicate that most men may have an oversimplified idea of the effort and duration involved in a timely and effective recovery. While many women who have sustained one or moreconcussions seem to doubt their recovery or want to protect themselves through limiting exercise or other potentially dangerous activities, men seem to bear few reservations about returning to physical activity post-injury. And, research has shown that maintaining a lower level of physical activity – if possible – can aid in the recovery process (see University of Buffalo’s 2013 study “Exercise treatment for postconcussion syndrome: a pilot study of changes in functional magnetic resonance imaging activation, physiology, and symptoms”).
This leads me to consider whether or not one’s cognitions can influence recovery speed. There are biological differences thatinfluence concussion incurrence rates and recovery in men (such as neck strength, which can affect the damage done to the brain upon impact), but psychological state may be crucial in regards to recovery as well. My questions: Is a healthy mental state essential for faster recovery? Do males with concussions tend to have healthier mental states than do females with concussions? If so, how and to what degree does this impact recovery? My personal observation dictates that many athletes who have ended their careers as a result of concussion buildup have experienced long-term depression and anxiety because of the sudden life change due to the incurrence of brain injury. I have especially noticed this in females. This is not to say that males do not experience these manifestations of psychological distress; rather, it is to insinuate that psychological elements of recovery seem to affect women to a more severe degree and for a longer duration.
For now, we can only hypothesize. The question of gender influences on concussion recovery is one that is currently being studied, and with the accelerating growth of the concussion field, there is much more to learn about gender, psychology, and outside factors that impact the recovery process. And of course, with the more that we learn, the more we discover there is to learn. There may be a large psychological component in recovery, and males may be predisposed to more easilyreframing cognitions surrounding this invisible injury. Certainly there should be research done on this in the future.
---
Arleigha Cook is a brain injury survivor and a former soccer player and sprinter for Trinity’s Womens’ soccer and track and field teams. After surviving her fourth concussion and receiving a diagnosis of Post-Concussion Syndrome, she has turned her focus to educating others about the effects of concussions. An English major with a concentration in creative writing, Arleigha started a blog, www.brainmatter4.blogspot.com, on which she posts her thoughts about her own personal experiences with brain injury. She has also been a guest blogger for B Stigma-Free and has spoken with Elite Sports Medicine at the Connecticut Children’s Medical Center about concussions, using her personal story as an example. Currently, she is over 1.5 years into her recovery.
Briana Scurry Guest Soccer Inspiration/Concussion Education
Mind Your Melon Invites
Youth Soccer Families to an Evening of
Soccer Inspiration and Concussion Education
with Special Guest Briana Scurry
Legendary US Goalkeeper
World Cup Champion
and Two Time Olympic Gold Medalist
Thursday, May 1, 2014
Sponsored by Shoreline Football Club
This event is pro-sport, upbeat and educational for young players from age 7 and up. Learn about the joys of soccer plus concussion education. Produced by Katherine Snedaker, MSW, the Mind Your Melon speakers don’t believe in scaring kids. We provide kids with helpful information to help make playing all sports safer.
3 PM Hangout with Briana @Location TBA in Darien/Stamford Briana and Katherine meet and chat with athletes with concussions or post concussion syndrome for a quiet, supportive 45 min talk – any age – no cost - Please RSVP with tickets here.
7-8 PM Soccer Inspiration and Concussion Education Event @Bluestreak Briana gives talk of inspiration and concussion education, plus local youth players/parents tell their stories followed by Katherine’s educational game “Concussion Simon Says.” General public, please buy tickets here. Shoreline Families have been sponsored by their Club and just reserve a free ticket.
Want a Ball signed by Briana for Your Child? The Education Event will end with Briana handing out up to ten pre-signed balls to raise funds to cover event expenses. Your child will be called up on stage to receive the ball from her, and be thanked as a supporter. Suggested donation of $200 for a soccer ball for Briana will sign with your child’s name and hers before the event. Please buy balls here BEFORE the event.
8:15-9 PM Intimate “Meet and Greet” Reception @BlueStreak (Total of 6 family tickets are available) Briana meets with kids and their families after the event. Dessert. Briana will sign photographs which we supply. Suggested donation of $400 for one family up to 5 members – Please buy tickets here.
Briana was a goalkeeper for the United States women’s national soccer team for most of the years between 1994-2008, earning a record 173 caps for the United States. She started 159 of those games and finished her international career with a record of 133-12-14. She also earned 71 shutouts.
Event would not be possible without support of our sponsors:
Bluestreak InjureFREE SoccerAndRugby and Fairfield County Sports Commission
Mind Your Melon is the youth outreach program of SportsCAPP.com
See all our websites for more information on Concussions
SportsCAPP.com Youth Sport Concussion Education for Players-Coaches-Parents
PinkConcussions.com Info & Research on all Types of Female Concussions
The Concussion Conference 2.0: RTL THEN RTP
One Day Concussion Management Training for School Nurses, School Staff and other Professionals who work with Concussed Students
The Concussion Conference 2.0
Wednesday, May 7, 2014 from 8 a.m. to 4 p.m.
Quinnipiac University School of Medicine | 370 Bassett Road | North Haven, CT
Due to the overwhelmingly positive response from 78 School Nurses, 25 MDs, and 25 ATs who attended the Jan 2014 Concussion Conferences and requests for more concussion management training, this new conference includes both:
- Advanced training with case studies for those who attended the 1st conferences to return for a higher level of study
- Basic foundation sessions for new participants
This conference will provide basic and advanced concussion management training for:
- School nurses
- School psychologists
- School guidance counselor/social workers
- School special education directors
- 504 Coordinators
- Athletic Trainers
- Physicians, PAs, and APRNs
See Flyer May2014 Concussion Conf_@QU(4)
Speakers for The May 7 Concussion Conference include nationally known experts and panels of local concussion professionals comprised of pediatricians, physical therapists, neuropsychologists, and advocates of brain injury prevention and athletic training education: Dr. Tricia McDonough-Ryan, Dr. Thomas Trojian, Katherine Snedaker MSW, Dr. David Wang, Dr. Mike Lee and the team of experts from Gaylord Center for Concussion Care, Representative from CATA; Deb Shulansky from Brain Injury Alliance of CT (BIAC); Brain Injury attorney and BIAC Board member Paul A. Slager; Charlie Wund, Founder & President Agency for Student Health Research; and Dr. Karissa Niehoff, The Executive Director at CT Association of Schools and CT Interscholastic Athletic Conference
Register now at TheConcussionConference.com - Early bird pricing until Monday, April 7
Event produced by Katherine Snedaker, PinkConcussions.com and SportsCAPP.com
Co-sponsored by Gaylord Center for Concussion Care
Each participant will be trained and will leave with a framework and materials needed to create a Concussion Management Team. The purpose of the CMTeam is to handle the 80% of concussions that resolve in the first month, based on research and nationally recognized best practices. For concussions that last beyond the 4 week period, academic accommodations will be taught which can be created in an IEP or a 504 plan for those students.
Early Morning Sessions are split between:
Foundation for First Time Participants
- Concussion 101 for School Staff and Medical Providers
- Concussion’s Impact on School: Strategies and Adjustments in the First 3 Weeks
- Time to Retire? Factors in a teen’s decision to retire from contact sports
Advanced Case Studies for Participants from 1st conference or Concussion Professionals
- Presentation of Case Study #1: A case from Gaylord Center for Concussion Care
- Presentation of Case Study #2: A case from Dr. Ryan and Kim Zemo, Social Worker
Late Morning and Afternoon Sessions for All Participants
- Existing Models of Concussion “Return to School” Plans in the USA and CT
- The Timing of Return to Learn (RTL), “Buffalo Protocol,” Return To Play in Student Athletes
- Beyond the Diagnosis: Eyes, Balance and Gait
- Post Concussion Syndrome: Depression, Isolation and Identity Loss, CTE Fact & Fiction
- Post Concussion Syndrome: Academic Modifications After One Month, Home Life Support
- New Research on “Does Concussion Education Work” and Concussion Resources
- The Past: State of CT Concussion Law and Development of Module #15
- The Present: CIAC’s Concussion Policy and Connecticut Law
Continuing Education Credits
- Gaylord Hospital is an Approved Provider of Continuing Nursing Education by The Connecticut Nurses’ Association, an Accredited Approver by the American Nurses’ Credentialing Center’s Commission on Accreditation. CNE application is pending for this program.
- This program has been submitted to The Commission for Case Manager Certification for approval to provide case managers pending clock hours.
- This activity is pending approval from the National Association of Social Workers.
- Program pending CME Activity approval via CT AAP.
Register now at TheConcussionConference.com
To participate as a conference sponsor or exhibitor, please contact Katherine at 203.984.0860 or Katherine@PinkConcussions.com
<May2014 Concussion Conf_@QU(4).pdf>
Guest post: 29 Fatality Cases of American Football Players in 2013
Originally posted at ChaneysBlog.com, currently offline. 29 Death Cases of American Football Players, 2013
Guest re-posting of Matt Chaney's Blog
Posted Sunday, November 17, 2013
Collision deaths of American high-school football players have increased markedly during 2013, suggesting this is not the year, once again, for “behavior modification” of modern ramming players who strike according to natural physics and the techno force of bullet-head helmets.
“Heads Up Football”—the latest version of old “head up” form theory for helmet-less hitting in forward-colliding sport, invalid through application attempts since the 1960s yet promised today by NFL commissioner Roger Goodell—has not prevented the fatal head and neck injuries of at least six high-school players this year, likely more pending further announcements of postmortem findings.
Below are 6 annotated cases of reported collision deaths among preps, followed by 3 possible collision fatalities of teen players for the year thus far, through Sunday, according to this blog’s ongoing review of critical gridiron casualty cases in Google information banks
By comparison, only one prep fatality involving collision was reported last year for tackle football, 2012 online: Dana Payne, 15, Tennessee, a running back drilled in a scrimmage, unable to rise afterward, whose cause of death was bronchial asthma with torso impact contributing, according to the Shelby County Medical Examiner’s Office.
An additional 7 cases below are apparently game-related player deaths during 2013, with no link to impact injuries per information available at this time; the fatal conditions apparently originated from physical exertion and more bodily stress during football-specific activities.
Finally, 13 cases of active player deaths reported during 2013 can neither be verified nor nullified for hard link to football, for a total collection below of 29 cases.
As usual, for electronic reviews since 2011, ChaneysBlog makes no scientific claim of case listings beyond raw information and disavows any qualification as football epidemiology.
Several limitations restrict injury reporting in vast American football, if not outright nullifying reliable collecting among millions of players mostly juvenile, particularly regarding the worst cases.
These annotated casualty cases of American football players are compiled strictly of information available in Google, primarily news reports, and require highly specialized follow-up for sound medical qualification.
These cases do not include 2013 deaths of active football players such as suicides, drug overdoses and more dangerous behavior outside competition and training. No deaths of coaches, referees and other field officials are included.
My heartfelt condolences to every one of the families below.
Deaths of Football Injuries Reportedly Involving Collisions
May 13: Jaleel Gipson, 17, Louisiana, a running back for Union Parish High School, sustained a fractured cervical vertebra while colliding in the head-on “Oklahoma Drill” during spring football practice on May 9. Four days later, Gipson was removed from life support and pronounced dead at hospital. “The injury occurred during a tackling drill,” reports Monroe sportswriter Cody Futrell. “Gipson was the ball carrier, and the coaching staff said he and the tackler used proper technique.” The school principal, David Gray, also contends that Heads Up theoretical technique, headless hitting, avoiding initial contact even by facemask, ruled a collision between players charging head-on that left one with a fatal broken neck. “Jaleel was carrying the football. He was head up in the exact position he needs to be,” Gray says. “The tackler led with shoulder as textbook, as taught and just an extremely unfortunate circumstance occurred. Tragic, a very tragic situation.” No video of the injury in practice was available online at time of this posting.
Aug. 16: De’Antre Turman, 16, Georgia, defensive back/receiver for Creekside High School, suffered fracture of the C3 vertebra while making a tackle during a scrimmage. “Tre broke on [the ball carrier], dislodged the ball and his body just went limp,” says witness Glenn Ford, who coached Turman in offseason training. The teenager, a recruit of the University of Kentucky, was later pronounced dead at hospital. “It was a fundamental tackle,” Ford says. “[Turman’s] head was up. It was a clean tackle. It was a clean tackle. He went down. Only God knows. You know, only God knows what happened.” No video of the scrimmage tackle was available online at time of this posting.
Aug. 28: Tyler Lewellen, 16, California, collapsed on sidelines during a scrimmage on Aug. 22, suffering a severe brain bleed. A CT scan revealed trauma and cerebral swelling and Lewellen remained comatose in ICU for five days, until life support was removed and he died soon after. Family members say doctors speculated whether the injury was a “second impact” from a previous undiagnosed concussion. Coaches say no clear evidence of a fatal head impact exists on video of the scrimmage, and on his last play Lewellen struck a ball carrier “with what appeared to be a glancing blow of the shoulder,” reports The New York Times. Autopsy results or video of the full scrimmage were not available online at time of this posting.
Sept. 16: Damon Janes, 16, New York, running back for the Westfield-Brocton “combined” team between two small high schools, suffered severe brain bleeding during a game on Sept. 13 and died three days later at hospital. Teammates, family members, other parents and news media say Janes was injured by a helmet-to-helmet hit in the game’s third quarter. Meanwhile, Gary Swetland, coach of the opposing team, Portville High, said his review of game video found “no obvious play that would lend one to think that a catastrophic injury was occurring or would occur,” reports The Buffalo News. The Westfield-Brocton team’s remaining football season was cancelled following the tragedy. Final autopsy results and complete game video involving the injury were not available in Google at time of this posting.
Oct. 6: Dylan Jeffries, 17, West Virginia, a running back/defensive back for South Harrison High School, suffered a “massive blood clot” of the brain during contact in a football game on Sept. 27. Emergency surgery relieved pressure and Jeffries was placed in a medically induced coma, but he died after nine days hospitalized. Family friend Mileena Beety wrote online: “To the Lincoln football team: Dylan knew many of you and was very excited about this game. Please do not blame yourselves if you tackled him or came in any contact with him throughout the game. He would have done the same to you if you were carrying the ball.”
Nov. 11: Charles Youvella, teenager, Arizona, a senior running back/defensive back for Keams Canyon Hopi High School, suffered severe brain bleeding during a game and died two days later at hospital. “Midway through the fourth quarter [with his team trailing 60-6], Youvella caught a pass followed by what officials said appeared to be a typical football tackle. On the way down, the back of Youvella’s head hit the ground hard,” report Chris Williams and Richard Obert for AZCentral.com. Autopsy results were unavailable on Google at time of this posting.
Football Deaths Possibly Involving Collision, American Football 2013
Oct. 12: Dodi Soza, 16, a running back for Downey High School, collapsed during a football game on Oct. 10 and died two days later at hospital. Soza had just scored a touchdown when he fell stricken, and initial reports of the casualty were of a possible cardiac arrest; later, Soza was reported to have sustained a brain injury. No confirmation or video of a collision injury was available in Google at time of this posting, nor were final autopsy results.
Oct. 29: Jacob Vick, 15, Virginia, a linebacker for New Kent High School, collapsed during football practice and later died at hospital. New Kent coach Dan Rounds said the starting varsity linebacker had just returned to play following diagnosed brain trauma: “Rounds said Vick recently sat out a game after sustaining a concussion, but received medical clearance to play in [the Oct. 25] game against Lafayette. Rounds said that after consulting with Vick’s parents, he did not play Vick in the game against Lafayette,” reports Marty O’Brien for The Newport News Daily Press. Autopsy results were unavailable in Google at time of this posting.
Nov. 14: Chad Stover, 17, Missouri, a football player for Tipton High School, suffered severe brain bleeding during a game on Oct. 31. Emergency surgery was performed and Stover remained comatose until dying two weeks after the injury. Autopsy results were publicly unavailable at time of this posting, and any evidence of football’s causing the brain hemorrhage remains unclear. An anonymous news source says Stover “had an undiagnosed preexisting medical condition, which may have been triggered by his participation in a contact sport,” reports KRCG-TV.
Player Deaths Involving Exertion or Stress of Football-Specific Activity
Jan. 5: Chandler Williams, 27, wide receiver for the Tampa Bay Storm, of the Arena Football League, collapsed while competing in a flag-football tournament, dying of cardiac arrest. Williams formerly played in the National Football League.
Aug. 3: Evan Raines, 16, North Carolina, a lineman for Seventy-First High School, experienced breathing problems after sprints to end football practice. Responders treated Raines for possible heat illness before he was transported to a hospital, where he later suffered cardiac arrest and died.
Aug. 7: Mitchell Cook, 14, California, a football player at Canyon High School, collapsed during warm-up drills at practice and was pronounced dead at hospital, apparently of cardiac arrest. Family members said Cook had a pre-existing heart condition that wasn’t considered life-threatening.
Aug. 16: Kaylan Carter, 16, California, a running back/defensive back for Enochs High School, collapsed of cardiac arrest during a weight-training session at the school on June 24. Carter remained comatose in ICU until life support was removed seven weeks later, and he died soon after.
Sept. 25: Jake West, 17, Indiana, a linebacker for LaPorte High School, suffered cardiac arrest during football practice and was later pronounced dead at hospital. An autopsy revealed “right ventricular cardiomyopathy,” reports WNDU-TV.
Oct. 4: Andre Maloney, 17, Kansas, a defensive back/receiver for Shawnee Mission West High School, suffered a cerebral stroke during a game on Oct. 3 and died the next day at hospital. Maloney, a recruit of the University of Kansas, had just scored a touchdown when he collapsed along a sideline.
Nov. 1: Caleb Allridge, 16, Louisiana, a lineman for Covenant Christian Academy, collapsed at home and later died at hospital, of a pulmonary embolism. His brother, Wilfred “PJ” Allridge III, said Caleb had been sidelined for weeks because of a knee injury in football: “Caleb was recovering from a dislocated knee injury that forced him to miss several football games this season, and PJ said swelling from the injury ended up causing an undetected blot in his heart and lungs,” reports Chris Singleton for HoumaToday.com.
Additional Deaths of American Football Players, 2013 To-Date
Jan. 15: Toron Murphy Jr., 17, Michigan, an offensive lineman for Martin Luther King Jr. Senior High School, collapsed after arriving at school in the morning and was pronounced dead at hospital, of cardiac arrest, dilated cardiomyopathy.
Jan. 21: Serxho Guraleci, 22, Michigan, senior defensive lineman for Wayne State University, collapsed during a weight-lifting session with teammates, dying of a heart attack “caused by a blood clot or hardening of the arteries typically from high cholesterol that a doctor says more than likely was genetic,” reports The Macomb Daily News. Guraleci had recently completed four seasons of football for Wayne State.
Feb. 2: Parker Allred, 16, Utah, football player and water polo player for Timpview High School, died of complications from staph infection and influenza.
Feb. 14: Xavier Walton, 20, Indiana, defensive lineman for Anderson University, collapsed while playing intramural basketball, suffering loss of heartbeat, and was pronounced dead at hospital. No autopsy results were available online at time of this posting.
Feb. 27: Falobi Akanbi, 17, Texas, an offensive lineman recruit for Montana State University, collapsed while playing pickup basketball and later died at hospital. Akanbi was a senior at Dawson High School in training for college football.
March 23: Michael Raybourn, 16, Missouri, a lineman for Excelsior Springs High School, died during sleep at his home.
June 26: Chad Stamper, 15, Minnesota, a football player and wrestler in training for Mora High School, died “of heart failure attributed to a pre-existing heart defect,” reports The Kanabec County Times.
Aug. 10: Sam Woodruff, 15, Utah, an offensive lineman for Grand County High School, died at home in the afternoon, during summer two-a-day practices. The team had practiced the previous night and that morning, and Woodruff was readying to attend evening practice when family members found him in a bathtub of running water, unresponsive. Woodruff had expressed concern for his weight and health to teammates, and family members suspected a heart problem affected him. No autopsy results were available online at time of this posting.
Sept. 15: Cameron Espinosa, 13, Texas, a lineman for Haas Middle School, suffered allergic reaction to ant bites during a game on Sept. 11, with the insects occupying mounds across the field of the Corpus Christi Independent School District. Espinosa died after four days hospitalized. Such casualties as the Espinoza tragedy are sometimes qualified as football-related, like the death of 11-year-old Jesse Watlington last year in Florida, caused by a lightning strike before team practice at Southwest Florida Christian Academy.
Sept. 27: Cameron Smith, 13, Kentucky, a lineman for Campbellsville Middle School, died suddenly at his home. “The Kentucky Middle School Football Association said Cameron Smith just stopped breathing,” reports WHAS-TV.
Oct. 22: Elijah Allen, 11, California, collapsed while playing football during recess at Vista Heights Middle School and later died at hospital. Some students say Allen was tackled as he went down, but teachers and school administrators say only a game of touch football was in progress. A pre-existing medical condition might have contributed to the death.
Oct. 23: Chase Watson, 15, Ohio, a receiver for Marlington High School, collapsed while jogging with a friend after football practice that afternoon. Watson was pronounced dead at hospital. Final autopsy results were not available in Google at time of this posting.
Nov. 5: Kylin Polhill, 14, New Jersey, a lineman for Marist High School, collapsed while playing pickup basketball on Nov. 4, having “stopped breathing,” and died the next day. Autopsy results were unavailable in Google at time of this posting.
Male Athletes & Concussions
[wufoo username="pinkconcussions" formhash="qeuqnku03xy370" autoresize="true" height="1513" header="show" ssl="true"]
Launch of International Study of Male Athletes and Concussions
Press Release: Monday, November 2, 2013
Launch of International Study of Male Athletes and Concussions
Study of Female Concussions Launches 2nd Study, to explore Male Athletes’ Experiences with Concussions
Contact:
Katherine Snedaker, MSW, PinkConcussions.com / 203-984-0860 PinkConcussions@gmail.com
Dr. Jimmy Sanderson, Clemson University / 864-656-3996 jsande6@clemson.edu
Norwalk, CT – Media attention and public interest in sports concussion injuries has been increasing at a rapid rate. As a result, it is important for researchers and concussion advocates to enhance research efforts on this very important topic. To provide some insight on female concussions, we launched a research study in October 2013, which focused on female athletes from all sports, and their past and present experiences with concussions. Via social media tweets & posts about the study, 652 women contacted us to participate. Of the 597 women who were eligible to participate and sent a link to the survey, 538 women completed the forty question online survey. This research study was also was designed to explore female verses male athletes' experiences with reporting concussions, another salient avenue in the concussions dialogue, as many athletes do not report concussions willingly or are mis-diagnosed.
Now we are recruiting for a NEW IBR approved study of male athletes and their experiences with concussions in conjunction with our recent efforts to recruit female athletes to discuss their concussion experiences.
This research aims to explore reasons why male/female athletes would report or not report concussions and examine potential gender differences that can inform the athletic, medical, and academic communities.
Current and former male athletes are eligible for this study which will be conducted by researchers from Clemson University with the advocacy group, Pink Concussions. For this study, male athletes, age 18 and over, who are willing to participate can sign up now at PinkConcussions.com or click here. Participants will be emailed a link to a twenty-minute online survey about their experiences with sports and non-sport concussions and reporting concussions.
The research also will investigate male/female athletes' willingness to have genetic testing that may show links to the repair and recovery of brain cells after concussion. After finishing the survey, participants in the study can opt for an additional study and consider submitting DNA collected by a cheek swab to be tested for variants at the Apolipoprotein E (APOE) gene. Testing for certain genes has previously documented an association between specific genetic factors and outcomes from injuries such as concussion.
Apolipoprotein E is a protein that is important in the repair and recovery of brain cells that have been damaged due to concussion. The clinical studies point to a relationship between certain genetic signatures and poorer overall concussion response. While additional evidence is needed to better understand the relationship between APOE status and concussion outcomes, the American Academy of Neurology introduced APOE testing into concussion management guidelines this year.
This research will be beneficial in shedding light on and male female athletes’ experiences with concussions and reporting concussions. We hope the results of this research will help further concussion research by focusing on the communicative element present in this issue, and the results of the study will be helpful for athletes, parents, administrators, physicians, and advocates.
Co-Researchers in this study are Dr. Jimmy Sanderson and Dr. Melinda Weathers in the Department of Communication Studies at Clemson University, along with Ms. Katherine Snedaker, MSW, of PinkConcussions.com.
# # #
For more information about this study, help in recruiting athletes or to participate in the study, please fill the contact form at PinkConcussions.com or contact:
Dr. Jimmy Sanderson Clemson University jsande6@clemson.edu 864-656-3996Katherine Snedaker PinkConcussions.com PinkConcussions@gmail.com 203-984-0860
Why birth control pills help a concussion + Why you should care
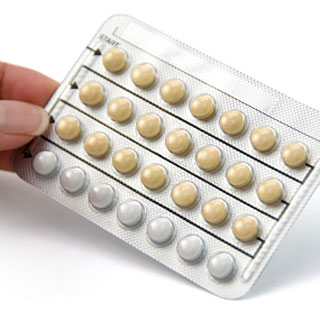 The recently published study, "Menstrual Phase as Predictor of Outcome After mTBI in Women" is so exciting because this study goes a step beyond confirming that women's concussions are different than men's. This research explored why in detail the differences occur within the subset of women themselves compared to men's experience of concussion.
The authors of the study are Kathryn Wunderle, BA; Kathleen M. Hoeger, MD, MPH; Erin Wasserman, BA; Jeffrey J. Bazarian, MD, MPH, of The University of Rochester.
The recently published study, "Menstrual Phase as Predictor of Outcome After mTBI in Women" is so exciting because this study goes a step beyond confirming that women's concussions are different than men's. This research explored why in detail the differences occur within the subset of women themselves compared to men's experience of concussion.
The authors of the study are Kathryn Wunderle, BA; Kathleen M. Hoeger, MD, MPH; Erin Wasserman, BA; Jeffrey J. Bazarian, MD, MPH, of The University of Rochester.
The Questions
Many of us who have experienced concussions or worked with women with mTBI have long felt there was a connection between concussion and a woman's cycle. In this study, researchers sought to prove the “Withdrawal Hypothesis,” which states that if a woman has a high level progesterone in her body at the time of an injury, she will experience sudden drop in progesterone. And that it is this decrease or "drop" that will cause worse concussion outcomes than a woman who had low level of progesterone at the time of injury and did not experience this "drop."
So who has a low level of progesterone (thought to be beneficial at the time of a concussion)?
- Men always naturally have low progesterone.
- Girls do before they get their first period.
- Women do, in later life, after their periods have ended.
Who has a high level of progesterone?
- Women of child-bearing years who progesterone levels rise and fall depending on the week of their cycle.
Researchers in this study hypothesized that women who experience mTBI during part of their cycles when progesterone is high, would have worse outcomes than women injured during time in their cycles when their progesterone is low.
Does anyone has level of progesterone which is resistant to this "drop?"
- Women taking birth control do not experience a drop as the pill provides constant high levels of synthetic progestins.
Remember in the case of this study, low progesterone levels at the time of concussion were predicted to be beneficial as they did not "drop" because they were low at the start. High levels which were subject to the "drop" were thought to predict poor outcomes.
The Answers
The final results of this study support the researchers' prediction that women in their cycle where "progesterone is highest, had worse post-concussion symptoms" than women whose progesterone is initially low. Similarly, women who were taking synthetic progestin as birth control seemed to mirror the women who were in the low progesterone phases.
The authors of the study warn that their findings must be "considered preliminary." Yet, they believe if their conclusions are "confirmed by others, it has important implications for both treatment and prognosis."
My mind races with the possibilities...
- Could this study be the starting point for a future hormone screening test - or even for a doctor to ask a simple question about when was an injured woman's last period?
- Could this simple screen alert doctors which women are more at risk and need more aggressive interventions?
- Could women in these risk groups based on their cycles be treated with progesterone after TBI?
As with every finding in the concussion field, more research needs to be done. But this study supports the hypothesis that the acute withdrawal of progesterone after mTBI may be the missing link (or one of the missing links) to why differences are seen in men and women's concussions. And in my opinion, this is a huge news for the concussion world - for men and women alike.
Objective: To determine whether menstrual cycle phase in women at the time of mild traumatic brain injury (mTBI) predicts 1-month outcomes.
Setting: Six emergency departments; 5 in Upstate New York, and 1 in Pennsylvania.
Participants: One hundred forty-four female participants (age, 16-60) who presented to participating emergency departments within 4 hours of mTBI.
Design: Nested cohort study with neurologic and quality-of-life outcome assessment, 1 month after enrollment. Female subjects aged 16 to 60 enrolled in the parent cohort study, with 1- month neurological determination data available, were classified into menstrual cycle groups by serum progesterone concentration and self-reported contraceptive use. Main Measures: Rivermead Post Concussion Questionnaire and EuroQoL/EQ5D.
Results: Women injured during the luteal phase of their menstrual cycle, when progesterone concentration is high, had significantly lower EuroQoL General Health Ratings and Index Scores than women injured during the follicular phase of their cycle or women taking oral contraceptives. Multivariate analysis confirmed a significant independent effect of menstrual cycle phase on EuroQoL Index Score and the Rivermead Post Concussion Questionnaire Somatic Subscore.
Conclusion: Menstrual cycle phase and progesterone concentration at the time of mTBI affect 1-month quality-of-life and neurologic outcomes. This association has important implications for treatment and prognosis after mTBI. Key words: brain concussion, brain injuries, follicular phase, luteal phase, menstrual cycle, postconcussion syndrome, progesterone, quality of life
PDF of The Menstrual Phase as Predictor of Outcome After mTBI in Women Study
Thank you to the authors - Kathryn Wunderle, BA; Kathleen M. Hoeger, MD, MPH; Erin Wasserman, BA; Jeffrey J. Bazarian, MD, MPH - and Leslie Orr of University of Rochester Medical Center - for allowing us to post this study.
Please direct questions to pricesned@gmail.com if you would like to take part in our exchange with the authors of the study.
NFHS responds to the IOM/NRC Concussion Report
After reading the IOM Concussion Report yesterday which put the NCAA and the NFHS in a leadership role, I called the NFHS to see what they thought about the report and how they viewed their role in the future.
I left a message for Bob Colgate, Director of Sports and Sports Medicine, National Federation of State High School Associations (NFHS) and Bob called me back today. I appreciate Bob taking the time to speak to me on a number of aspects about concussion including the online NFHS Concussion Training Course and NATIONAL HIGH SCHOOL SPORTS-RELATED INJURY SURVEILLANCE STUDY. We both agreed on the importance of concussion education for coaches, parents, school staff, and students - all students - not just student-athletes.
Bob then emailed me with the following press release: NFHS Responds to Concussion Report. Please see my follow-up questions/comments following the press release.

INDIANAPOLIS, IN (November 1, 2013) — On October 29, the Institute of Medicine (IOM) and the National Research Council (NRC) released a detailed report on “Sports-Related Concussions in Youth – Improving the Science, Changing the Culture.”
The National Federation of State High School Associations (NFHS), which has been a leader among national sports organizations in the area of concussion awareness and management the past five years, fully cooperated with the preparation of the report and is in support of many of the report’s recommendations.
“We support the report’s conclusion that a culture change is a national priority,” said Bob Gardner, NFHS executive director. “Concussions are not ‘dings’ – they are serious medical conditions that need to be addressed. I am pleased to report that the NFHS places its highest priority on risk minimization for the 7.7 million participants in high school sports.”
In 2008, the NFHS Sports Medicine Advisory Committee advocated that a concussed athlete shall be immediately removed from play and not return until cleared by an appropriate health-care professional. For the past four years, all NFHS rules publications have contained guidelines for the management of an athlete exhibiting signs, symptoms or behaviors consistent with a concussion.
In addition, with help from the Centers for Disease Control (CDC), the NFHS developed a free, 20-minute online course “Concussion in Sports – What You Need to Know.” More than 1.2
million administrators, coaches, officials, athletes, parents and health-care professionals have taken the course since 2010. (See www.nfhslearn.com)
The NFHS also agrees that injury surveillance is important to help prevent future injuries. Since 2005, the National High School Sports-Related Injury Surveillance Study (High School RIO), commissioned by the NFHS and compiled by Dr. Dawn Comstock, principal investigator from the Pediatric Injury Prevention, Education and Research (PIPER) program at the Colorado School of Public Health and Colorado Children’s Hospital in Aurora, Colorado, has been collecting injury surveillance data for the NFHS. (visit http://www.ucdenver.edu/academics/colleges/PublicHealth/research/ResearchProjects/piper/projects/ RIO/Pages/Study-Reports.aspx for the full reports.)
The NFHS also works with the National Center for Catastrophic Sports Injury Research (NCCSIR) at the University of North Carolina-Chapel Hill, which has been collecting catastrophic injury data on all sports for more than 35 years.
“The NFHS strives to minimize risk for all high school athletes in all sports,” Gardner said. “The athletic community – administrators, coaches, officials, athletes, parents and health- care professionals – should know that this support system of rules, education and research exists to provide a safer environment for all athletes in all sports. We hope the report will encourage all these leaders in the high school athletic community to recognize and respond more effectively to concussions.”
### About the National Federation of State High School Associations (NFHS)
The NFHS, based in Indianapolis, Indiana, is the national leadership organization for high school sports and performing arts activities. Since 1920, the NFHS has led the development of education-based interscholastic sports and performing arts activities that help students succeed in their lives. The NFHS sets direction for the future by building awareness and support, improving the participation experience, establishing consistent standards and rules for competition, and helping those who oversee high school sports and activities. The NFHS writes playing rules for 17 sports for boys and girls at the high school level. Through its 50 member state associations and the District of Columbia, the NFHS reaches more than 19,000 high schools and 11 million participants in high school activity programs, including more than 7.7 million in high school sports. As the recognized national authority on interscholastic activity programs, the NFHS conducts national meetings; sanctions interstate events; offers online publications and services for high school coaches and officials; sponsors professional organizations for high school coaches, officials, speech and debate coaches, and music adjudicators; serves as the national source for interscholastic coach training; and serves as a national information resource of interscholastic athletics and activities. For more information, visit the NFHS Web site at www.nfhs.org.
Bruce Howard, 317-972-6900 Director of Publications and Communications National Federation of State High School Associations bhoward@nfhs.org
Chris Boone, 317-972-6900 Assistant Director of Publications and Communications National Federation of State High School Associations cboone@nfhs.org
Questions I have after reading the release and have emailed Bob Colgate for clarification:
1. From this statement, "The National Federation of State High School Associations (NFHS)... fully cooperated with the preparation of the report and is in support of many of the report’s recommendations," can I take that the NFHS doesn't completely agree with "all" the recommendations?
What parts of the IOM report are not supported by the NFHS and which are supported by the NFHS?
2. I read the IOM committee's recommendation that the "NCAA and NFHS (in conjunction with others..) develop, implement, and evaluate" as if the current efforts of concussions education/training/research efforts are not enough, and in the future, the NCAA and NFHS would lead the way with new "large-scale efforts."
The statement from NFHS press release states all that the NFHS has done (which is very commendable) but it "appears" by saying "We hope the report will encourage all these leaders in the high school athletic community to recognize and respond more effectively to concussions,” seems that the buck is passed to the high schools themselves.
Is the NFHS going to initiate any new programs or initiatives based on what was learned in the IOM report?
Is there anyway for the NFHS to hold high schools accountable or reward the schools to make the changes needed?
...
We have been waiting for a year the IOM report and the APP report which is a clear blueprint for schools to follow. So now with these reports in hand along with the various concussion online trainings, and variety of education flyers, who is going to lead the way and how?
The IOM recommends the NCAA and NFHS as for the job of leading schools and sports organizations. The NFHS press release states what they have already been doing.
What can the NFHS really do beyond supplying its members with info (which they have already done) and funding the data collection of injury rates (which they are doing)?
I realized it is a balancing act for organizations which rely on voluntary members to require/demand their membership meet certain standards. I have talked with Steve Stenersen, President of US Lacrosse, over the years on the issues of carrot or stick with concussion education/training and youth lacrosse organizations. There are really no sticks to use with members who can leave your organization, and carrots cost money.
Note: From my read, the IOM Report does not suggest any source of funding for any organization to use to pay for any of the recommendations the report suggests. It is hard to be passed the command without the funds to pay the troops.
- Could there be an answer in the NFHS accrediting a high school with a NFHS "concussion-prepared," or "concussion-savy" stamp of approval when a school hires full time ATs and trains coaches, staff, parents and students?
- Could a seal of approval from the NFHS be something for the schools to strive for to be the "highest level" of prepared a school can be (in the concussion field which is still developing)?
- Would parents value this standard and pressure schools who did not meet the standard?
Concussion education isn't hard to understand, and the resources exist to teach coaches, parents and students. What is missing is the commitment of overburdened schools, sports organization and parents to make the time to attend the classes or complete the online trainings or read the flyers. We need leaders now find ways to ensure education takes place, to encourage individual states to update their concussion laws with mandatory requirements, and find sources of funding so the needed research is done.
Good News, Bad News in long awaited Nat'l Concussion Reports
Reblogged from www.SportsCAPP.com Good News...
The IOM and the National Research Council formed an expert committee to review the science of sports-related concussions in youth from elementary school through young adulthood, as well as in military personnel and their dependents. The committee’s report recommends actions that can be taken by a range of audiences – including research funding agencies, legislatures, state and school superintendents and athletic directors, military organizations, and equipment manufacturers, as well as youth who participate in sports and their parents – to improve what is knows about concussions and to reduce their occurrence.
The report finds that while some existing studies provide useful information, much remains unknown about the extent of concussions in youth; how to diagnose, manage, and prevent concussions; and the short- and long-term consequences of concussions as well as repetitive head impacts that do not result in concussion symptoms.
Bad News... There is no mention of any funding.
Good News... Here is who sponsored the IOM Report:

Bad News? Here is who the IOM Committee recommends to lead the effort...
Interesting neither group helped sponsor the study?
NCAA is not well thought of by many concussion field. In March, I had a face to face conversation with Mark Emmert NCAA President where I asked about limiting full contact practice in the NCAA schools to match the NFL and Ivy Schools reduced schedule, and he told me there wasn't enough evidence and there needed to be more studies before he felt he could act. I am wondering if the many lawsuits are helping to motivate him to move on something here?
I am going to contact the NFHS and ask how they see their role in the future. Here is what the NFHS said.
Good News... We now have a National Sports Concussion Coalition.
Bad News... This coalition was not mentioned in the IOM Report.
So in summary...
Good News... This week we do have two new reports - a very informative the IOM Concussion and Youth Sports Report with ideas and recommendations along with the new road map for schools in APP report on Concussions and Schools.
Bad News... There doesn't seem to be any funding mentioned in either report to fund any of these recommendations.



















